Clinical profile and management outcomes of Intussusception in children in Uyo, South-South, Nigeria.
Main Article Content
Abstract
Background: Intussusception is the most common cause of intestinal obstruction in infants and children in Sub-Saharan Africa, and it is frequently associated with significant morbidity and mortality if treatment is delayed.
Objective: To investigate the presentation, management, and outcomes of paediatric intussusception at the University of Uyo Teaching Hospital over a 10-year period.
Materials and Methods: This retrospective, descriptive study examined children diagnosed with intussusception from January 2014 to December 2023. Data were collected from case notes and included patient’s demographics, clinical presentation, surgical procedures, intraoperative findings, and postoperative outcomes.
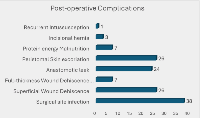
Results: A total of 180 patients were included, comprising 103 males and 77 females (male-to-female ratio: 1.33:1). Ages ranged from 2 months to 5 years (median: 6 months, IQR 5 – 7months). Only 22 patients (12%) presented within 3 days of symptom onset. Idiopathic cases accounted for 97.2%. Ultrasonography confirmed the diagnosis in 77.8% of cases. Surgical treatment was required in 82.8% of patients, with ileocolic intussusception observed in 138 patients (76.7%). Manual reduction was performed in 38.3% of cases, while bowel resection was required in 44.4%. The overall complication rate was 40.0%, with surgical-site infections being the most common (21.1%). The mortality rate was 12.8%, with delayed presentation and reoperation identified as key predictors of mortality (p = 0.016 and 0.01, respectively).
Conclusion: Late presentation remains a significant challenge in managing intussusception in our setting, contributing to high morbidity and mortality. Surgical intervention is often necessary to manage these cases effectively.
Downloads
Article Details
Section

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.
The Journal is owned, published and copyrighted by the Nigerian Medical Association, River state Branch. The copyright of papers published are vested in the journal and the publisher. In line with our open access policy and the Creative Commons Attribution License policy authors are allowed to share their work with an acknowledgement of the work's authorship and initial publication in this journal.
This is an open access journal which means that all content is freely available without charge to the user or his/her institution. Users are allowed to read, download, copy, distribute, print, search, or link to the full texts of the articles in this journal without asking prior permission from the publisher or the author.
The use of general descriptive names, trade names, trademarks, and so forth in this publication, even if not specifically identified, does not imply that these names are not protected by the relevant laws and regulations. While the advice and information in this journal are believed to be true and accurate on the date of its going to press, neither the authors, the editors, nor the publisher can accept any legal responsibility for any errors or omissions that may be made. The publisher makes no warranty, express or implied, with respect to the material contained herein.
TNHJ also supports open access archiving of articles published in the journal after three months of publication. Authors are permitted and encouraged to post their work online (e.g, in institutional repositories or on their website) within the stated period, as it can lead to productive exchanges, as well as earlier and greater citation of published work (See The Effect of Open Access). All requests for permission for open access archiving outside this period should be sent to the editor via email to editor@tnhjph.com.
How to Cite
References
Ogundoyin OO, Afolabi AO, Ogunlana DI, Lawal TA, Yifieyeh A. Pattern and outcome of childhood intestinal obstruction at a tertiary hospital in Nigeria. Afr Health Sci. 2009;9(3):170-173.
Ooko PB, Wambua P, Oloo M, Odera A, Topazian H, White R. The spectrum of paediatric intestinal obstruction in Kenya. Pan Afr Med J. 2016;24(43).
Zewde Y, Bugie T, Daniel A, Wodajo A, Meskele M. Clinical presentation and management outcome of pediatric intussusception at Wolaita Sodo University Comprehensive Specialized Hospital: a retrospective cross-sectional study. J Int Med Res. 2024;52(3):3000605241233525.
Jiang J, Jiang B, Parashar U, Nguyen T, Bines J, Patel MM. Childhood intussusception : a literature review. PLoS One. 2013;8(7)
Barbette P. Ouevres Chirurgiques et Anatomiques. Geneva, Francois Miege; 1674:5221.
Hunter J. On introsusception. In: Palmer JF, ed. The Works of John Hunter. FRS London. London; 1837:587-593.
Columbani PM, Scholz S. Intussusception. In: Coran AG, ed. Pediatric Surgery. 7th ed. Mosby; 2012:1093-1110.
Akello VV, Cheung M, Kurigamba G, et al. Pediatric intussusception in Uganda: differences in management and outcomes with high-income countries. J Pediatr Surg. 2020;55(3):530-534.
IBM Corp. IBM SPSS Statistics for Windows, Version 24.0. Armonk, NY: IBM Corp; 2016.
Chalya P, Kayange N, Chandika A. Childhood intussusception at a tertiary care hospital in Northwestern Tanzania: a diagnostic and therapeutic challenge in resource-limited settings. Ital J Pediatr. 2014; 40:28.
Bode CO. Presentation and management outcomes of childhood intussusception in Lagos: a prospective study. Afr J Paediatr Surg. 2008;5(1):24-28.
Ekenze SO, Mgbor SO, Okwesili OR. Routine surgical intervention for childhood intussusception in a developing country. Ann Afr Med. 2010;9(1):27-30.
Ogundoyin OO, Olulana DI, Lawal TA. Childhood intussusception: a prospective study of management trend in a developing country. Afr J Paediatr Surg. 2015;12(3):217-220.
Tagbo BN, Ezomike UO, Odetunde OA, et al. Intussusception in children under five years of age in Enugu, Nigeria. Pan Afr Med J. 2021;39(Suppl 1):9.
Bwala KJ, Umar AM, Bashir MF, et al. Pattern, presentation, and management of intussusception at Abubakar Tafawa Balewa University Teaching Hospital, Bauchi, Nigeria. Ann Med Res Pract. 2022; 3:7.
Li Y, Zhou Q, Liu C, et al. Epidemiology, clinical characteristics, and treatment of children with acute intussusception: a case series. BMC Pediatr. 2023; 23:143.
Pandey A, Singh S, Wakhlu A, Rawat J. Delayed presentation of intussusception in children: a surgical audit. Ann Pediatr Surg. 2011;7(3):130-132.
Usang UE, Inah GB, Inyang AW, Ekabua AT. Intussusception in children: comparison between ultrasound diagnosis and operation findings in a tropical developing country. Afr J Paediatr Surg. 2013;10(2):87-90.
Ghritlaharey R. Management of intussusception secondary to pathological lead points in Nigerian children. Ann Natl Acad Med Sci. 2021; 57:53-57.
Yehouenou Tessi RT, El Haddad S, Oze KR, et al. A child's acute intestinal intussusception and literature review. Glob Pediatr Health. 2021;8.
Parker B, Blickman JG. Gastrointestinal Tract. In: Blickman JG, Parker BR, Barnes PD, eds. Pediatric Radiology. 3rd ed. Mosby; 2009:63-102.
Alazraki AL, Richer EJ. Pediatric Abdominal Pain. In: Milla SS, Lala S, eds. Problem Solving in Pediatric Imaging. Elsevier; 2021:98-126.
Marsicovetere P, Ivatury SJ, White B, Holubar SD. Intestinal intussusception: etiology, diagnosis, and treatment. Clin Colon Rectal Surg. 2017;30(1):30-39.
Aydin E, Beşer OF, Ozek E, Sazak S, Duras E. Is there a causal relationship between intussusception and food allergy? Children. 2017;4(10):89.
Chukwubuike KE. Assessment of the correlation between age of commencement of cereal feeds and childhood intussusception. Clin Surg J. 2021;4(S10):18-24.
Onofiok NO, Nnanyelugo DO. Weaning foods in West Africa: nutritional problems and possible solutions. Food Nutr Bull. 1998;19(1):27-33.
Aliyu I, Duru C, Lawal TO, Mohammed A. Breastfeeding and weaning practices among Nigerian women. J Med Investig Pract. 2014;9(4):140-143.
Kuremu RT. Childhood intussusception at the Moi Teaching and Reference Hospital, Eldoret: management challenges in a rural setting. East Afr Med J. 2004; 81:443-444.
Buettcher M, Baer G, Bonhoeffer J, Schaad UB, Heininger U. Three-year surveillance of intussusception in children in Switzerland. Pediatrics. 2007;120(3):473-480.
Belachew AG, Tadesse A, Bogale BH. Patterns and seasonal variation of intussusception in children: a retrospective analysis of cases operated in a tertiary hospital in Ethiopia. Ethiop Med J. 2016;54(1):14-18.
Madan AJ, Haider F, Alhindi S. Profile and outcome of pediatric intussusception: a 5-year experience in a tertiary care center. Ann Pediatr Surg. 2021; 17:31.
Wu TH, Huang GS, Wu CT, Lai JY, Chen CC, Hu MH. Clinical characteristics of pediatric intussusception and predictors of bowel resection in affected patients. Front Surg. 2022; 9:926089.
Rajkarnikar R, Singh S, Joshi MP, Kayastha A. Intussusception among children admitted in a department of pediatric surgery of a tertiary care centre: a descriptive cross-sectional study. JNMA J Nepal Med Assoc. 2023;61(258):150-153.
Kotloff KL. Abdominal Symptom Complexes. In: Long SS, ed. Principles and Practice of Pediatric Infectious Diseases. 6th ed. Elsevier; 2023:178-182.e1.
Charles T, Penninga L, Reurings J, Berry M. Intussusception in children: a clinical review. Acta Chir Belg. 2015; 115:327-333.
Abdulhai S, Ponsky T. Intussusception in infants and children. In: Wyllie R, Hyams J, Kay M, eds. Pediatric Gastrointestinal and Liver Disease. 6th ed. Elsevier; 2021:549-551.e1
Talabi AO, Sowande OA, Etonyeaku CA, Adejuygbe O. Childhood intussusception in Ile-Ife : What has changed ? Afr J Paediatr Surg. 2013;10(3):239-242.
Ajao AE, Lawal TA, Ogundoyin OO, Olulana DI. Clinical predictors and outcome of bowel resection in paediatric intussusception. Afr Health Sci. 2020;20(3):1463-1470.
Mpabalwani EM, Mwenda JM, Tate JE, Parashar UD. Review of naturally occurring intussusception in young children in the WHO African Region prior to the era of rotavirus vaccine utilization in the expanded programme of immunization. J Trop Pediatr. 2017;63(3):221-228.
Hedrick TL, Sawyer RG, Foley EF, et al. Anastomotic leak and the loop ileostomy: friend or foe? Dis Colon Rectum. 2006;49(8):1167-1176.
Ameh E, Ayeni M, Kache S, Mshelbwala P. Role of damage control enterostomy in management of children with peritonitis from acute intestinal disease. Afr J Paediatr Surg. 2013;10(4):315-319.
Akpanudo E, Ituen AM, Eyo A, Emmanuel E. Ileostomies for severely ill children with ileocolic intussusception: our experience at the University of Uyo Teaching Hospital. Ibom Med J. 2024;17(2):251-259.
Tesfaye DD, Adem BM, Ketema I, Mehadi A, et al. Clinical profile and treatment outcome of acute intussusception among children in eastern Ethiopia: a seven years’ retrospective study. Front Pediatr. 2022; 10:968072.
Ezomike UO, Nwangwu EI, Chukwu IS, Aliozor SC, et al. Trends in childhood intussusception in a Nigerian tertiary hospital. Afr Health Sci. 2024;24(1):213-219.
Sadigh G, Zou KH, Razavi SA, Khan R, Applegate KE. Meta-analysis of air versus liquid enema for intussusception reduction in children. Am J Roentgenol. 2015;205(5)
Cox S, Withers A, Arnold M, et al. Clinical presentation and management of childhood intussusception in South Africa. Pediatr Surg Int. 2021;37(10):1361-1370.
Adesanya OA, Aremo A, Adesanya OO. Childhood intussusception in Abeokuta, South-West Nigeria. J Clin Sci. 2020;17(2):20-23.
Ogundoyin OO, Afolabi AO, Lawal TA. Paediatric intussusception in Ibadan, Southwestern Nigeria. Niger J Surg. 2008;14(1):13-16.
Mpabalwani EM, Chitambala P, Chibumbya J, et al. Intussusception incidence rates in 9 Zambian hospitals 2007-2011: pre-rotavirus vaccine introduction. Pediatr Infect Dis J. 2014;33(Suppl 1)
GlobalSurg Collaborative. Determinants of morbidity and mortality following emergency abdominal surgery in children in low- and middle-income countries. BMJ Glob Health. 2016;1(4)
Talari K, Goyal M. Retrospective studies—utility and caveats. J R Coll Physicians Edinb. 2020;50(4):398-402.